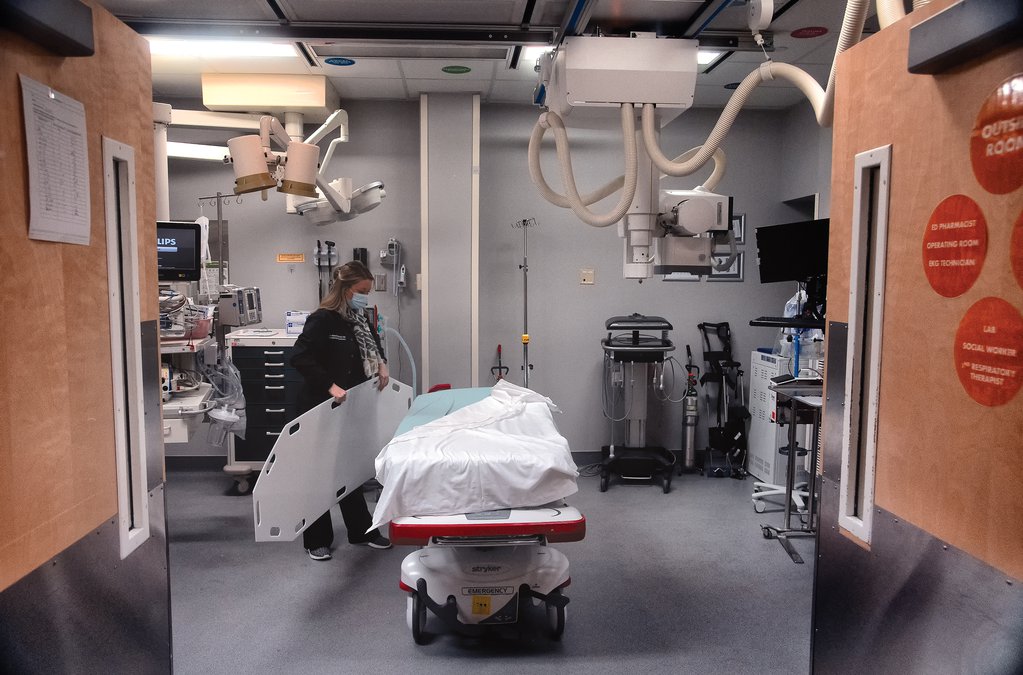
If you think your 2020 plans went out the window with COVID-19, spare a thought for a hospital trying to revamp its emergency department as part of a larger $700 million project.
How $700M plan for new ER, 11-story tower at hospital may benefit from COVID-19 lessons