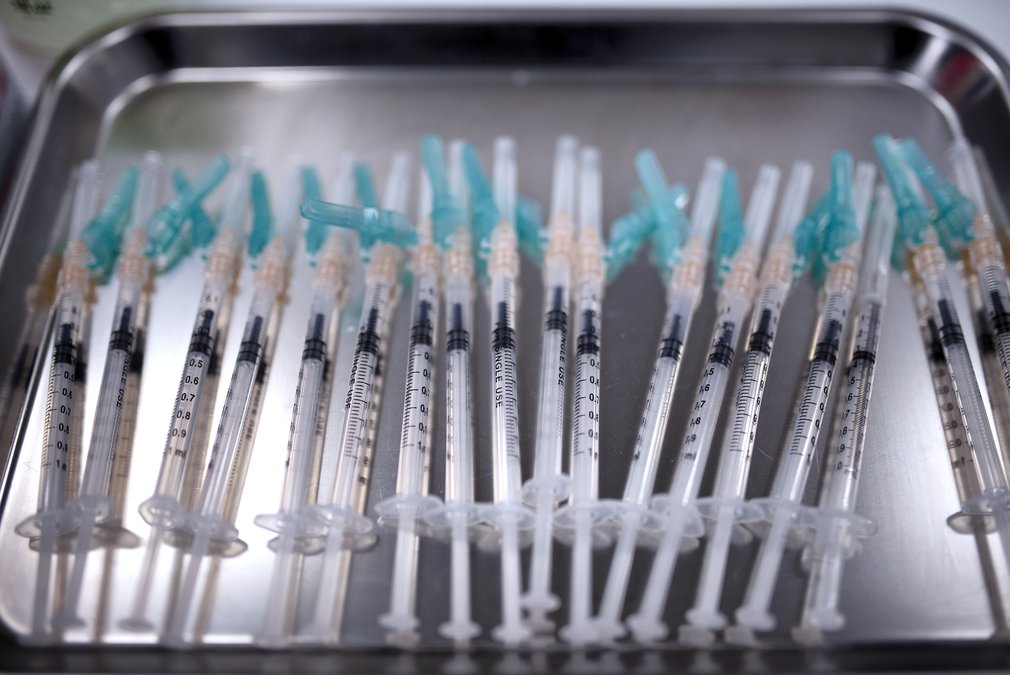
Since March 25, all Georgians ages 16 and up are eligible to receive doses of the COVID-19 vaccine.
Hesitant about getting the COVID-19 vaccine? Here’s what health officials say