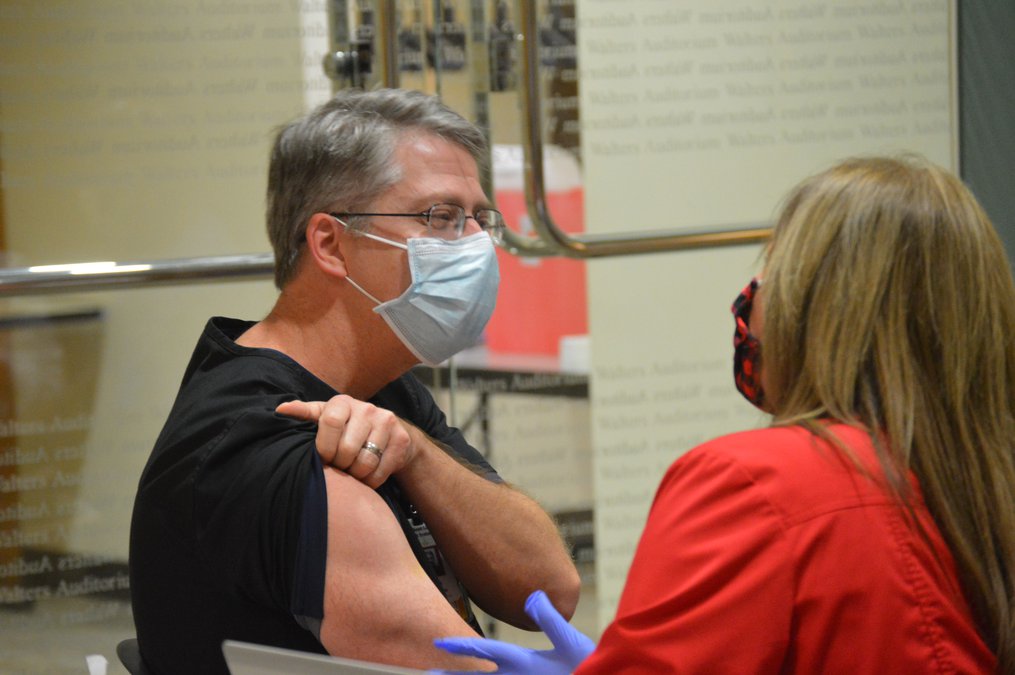
The Department of Public Health says health departments and some hospitals in Georgia are reporting roughly 30% of health care workers have received the COVID-19 vaccine.
Compliance, refusal or wait and see: About 30% of health care workers vaccinated so far